More than nine months after coronavirus vaccines were made available, inequities in Florida’s distribution process are still affecting some populations.
Though a majority of people who haven’t been vaccinated are white, vaccination rates among Black Floridians are still far behind their white and Hispanic counterparts.
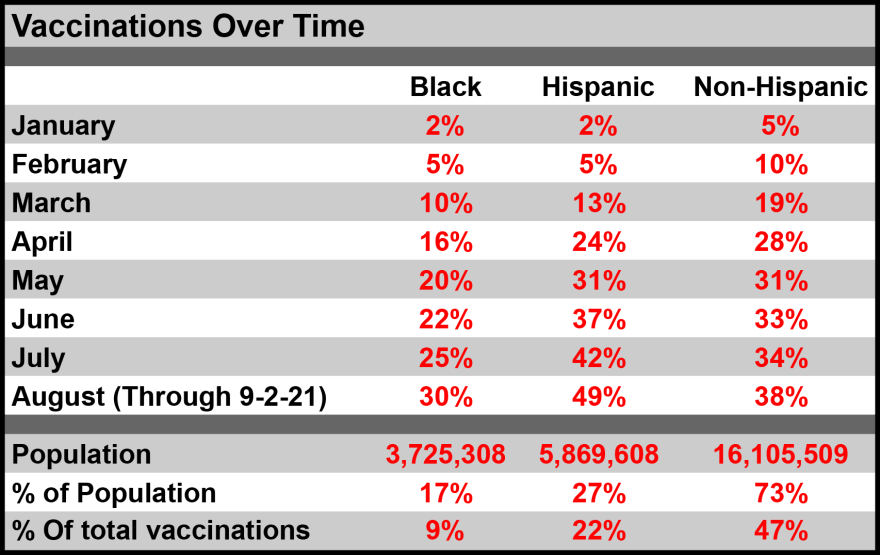
The state reports 49% of white people in Florida are vaccinated, compared with 31% of Black people.
And data from the Florida Department of Health shows just 9% of all vaccines delivered in Florida have gone to Black people, though they make up about 17% of the population.
But the data isn’t entirely complete. Both race and ethnicity information was missing for 13% of those who received a vaccination in Florida.
So how did we get here?
Inequities in Florida’s health care system are not new, but they’ve been magnified during the coronavirus pandemic and vaccine rollout.
“We have a 200-year history of health inequity and health disparities in this country, and we need to do away with that,” said Kevin Sneed, dean of the University of South Florida’s Taneja College of Pharmacy and head of WE-CARE, a group that aims to get more people of color involved in clinical research.
Sneed has spent much of the past year educating people about the vaccines and working to expand access to boost immunization rates among Black and Hispanic residents.
“And we’re at a moment now where we can’t look back after the fact and say how can we do better next time because for many of them there won’t be a next time,” he said early in vaccine rollout.
But it didn’t take long for barriers to access for people of color to appear.

"Seniors first"
Gov. Ron DeSantis put a priority on older people who are more likely to get sick and die of COVID-19 as soon as vaccines against coronavirus became available, in December 2020.
“When experts said put workers first, Florida put seniors first,” DeSantis said in January as vaccines were being rolled out at Publix grocery stores around the state.
Of course, the vaccine wasn’t just for white seniors. But Sarasota Dr. Lisa Merritt, who heads the Multicultural Health Institute, said the way Florida handled the initial rollout tended to favor people with education and money.

"There is such a disconnect from privileged people worried about how they can pay their way to get first in line for the vaccine, to the people on the ground who are just trying to find out where they are going to get their next meal," she said.
Seniors who got the vaccine early were those who could navigate the chaotic sign-up process, often helped by younger family members who secured appointments for them, said Deborah Austin of REACHUP, a Tampa-based organization that aims to help achieve equality in health care.
“You’ve got to have internet access, you've got to be able to sit there and wait,” Austin said. “I mean people have said even with the phone it took them 100 times. I mean you’ve even got to have time.”
More at risk
Data from the Centers for Disease Control and Prevention show that nationally, Blacks and Hispanics died from COVID-19 at twice the rate of whites and hospitalized at nearly three times the rate.

One of the challenges is that due to systemic inequities in health care, Black and Hispanic people were already more likely to have health problems that put them at a higher risk for severe COVID-19, said Angela Hill, who works with Sneed at USF’s College of Pharmacy and WE-CARE.
“So the hypertension, the diabetes, strokes, certainly even the dementia – all of those things predisposed Black and brown populations for ending up either on a ventilator or just having a harder experience,” Hill said.
Because of this, advocates say people of color needed to be prioritized for vaccinations.
DeSantis maintained that race wasn’t a factor in vaccine distribution. Seniors were the primary driver of his administration's vaccine efforts.
“Just to be clear there is not any kind of racial discrimination,” DeSantis said in January asked about the equity of pop-up vaccination sites. “They are not accounting for race. It is all based on age.”

But as more pop-up sites began to emerge, there was controversy about locations.
Like one that the governor hosted in Lakewood Ranch, a wealthy suburb in Manatee County in February. Three thousand vaccines were distributed to people in two specific ZIP codes with some of the highest income levels and lowest coronavirus rates in the area.
That sent a strong message to underserved communities, said Trevor Harvey, head of Sarasota’s NAACP chapter.
“It seems like you're setting these things up in communities who have less issues than communities of color and to us that shows racial disparities,” he said. “That shows classic racism.”
The state did not respond to several requests for comment and information about initiatives to vaccinate underserved communities.
But in a response to another WUSF story, DeSantis spokeswoman Christina Pushaw said the governor has spent more time this year on expanding access to vaccines for “all eligible Floridians,” than on any other policy priority.
Grass-roots effort
Community advocates played a large role in organizing smaller vaccination events, at places like Black churches. The Florida Department of Health would supply the vaccines and staff. Advocates would provide the venue and recruit people to come get their shots.
At an event at Sarasota’s Light of the World International Church in February, Franklin Cochran, 78, was among those getting the shot. He recently had hip surgery and didn’t want to miss the opportunity.
“Because we want to live a long time, and this is our best shot right here,” Cochran said.
Cochran said he doesn’t feel comfortable driving long distances so he appreciated having the site at the church in his community. He said he knew there were racial disparities in the COVID vaccine rollout, and hoped events like this raised awareness.
“Because Blacks and Hispanics, we catch hell, and that's on every level of society,” Cochran said.
Door to door
By spring, the state harnessed the single-dose Johnson & Johnson vaccine to host more frequent pop-up sites in underserved communities to address some of the equity issues.
The Florida Division of Emergency Management deployed canvassers to go door to door in neighborhoods and visit local parks and supermarkets.
They talked with people about the vaccines, sometimes in Spanish.
Canvassers spread the word about these mobile sites and helped people register for appointments on the spot, said Stacey Gedeon who led a team in Hillsborough County.
“To help break down that barrier and make the vaccine really accessible to everyone who actually wants it,” Gedeon said.
Community groups led similar initiatives, with some hosting their own pop-ups and even doing homebound vaccinations.

All of these efforts have helped thousands more Black and Hispanic residents get vaccinated this year, and their rates keep on improving.
State data show vaccination rates among whites and Hispanics are pretty much even now.
But it shows white Floridians are still more than 1.5 times more likely as Black residents to be vaccinated.
Advocates like Sarasota’s Dr. Washington Hill are trying to close that gap. He goes out into the community and encourages people to get vaccinated. He recalled one event at a farmers market that only distributed a handful of vaccinations.
“We've been out here six hours, and it's hot, we only did six,” Hill said. “And I say, you know that’s six people who would not have gotten the vaccine if we'd not been here.”
Even though progress can inch along at times, Hill said, it’s worth it.
Coming up: The next parts in our Unequal Shots series will take a deeper look at some of the barriers that have made it more challenging for some Black and Hispanic residents to get vaccinated -- and we’ll highlight successful efforts to overcome those hurdles and improve vaccine equity.
9(MDAyNDY5ODMwMDEyMjg3NjMzMTE1ZjE2MA001))
Our stories reflect reporting within the community, public records requests and other interviews designed to put the pandemic and health disparities in context. We’ve reached out to government and official sources and let you know when information we requested was not provided, or if sources declined interview requests.
Kerry Sheridan is an award-winning reporter and co-host of All Things Considered at WUSF Public Media. She covers education, health and science. Prior to joining WUSF in 2019, Kerry reported for Agence France-Presse from 2005 to 2019, reporting from the Middle East bureau in Cyprus, followed by stints in Washington and Miami. Kerry earned her master’s degree from the Columbia University Graduate School of Journalism in 2002, and was a recipient of the Pulitzer Traveling Fellowship for Cultural Reporting.
Julio Ochoa is an assistant news director at WUSF and the award-winning editor of Health News Florida, a collaborative statewide news project. He also reports on health care with a focus on policy. Prior to joining WUSF in 2015, Julio worked at the Tampa Tribune, where he began as a website producer for TBO.com and served in several editing roles, eventually becoming the newspaper’s deputy metro editor.
Copyright 2021 WUSF Public Media - WUSF 89.7





